ATP Bioenergetics, Fatigue Depression in Young Adults
Led by Kathryn Cullen, a research team at the University of Minnesota, the University of Queensland, and the Mayo Clinic studied depression and fatigue in young adults with and without early-stage depression. They found a positive correlation between ATP levels and levels of depression in young adults that correlates with depression and suggests a compensatory mechanism early in the disease. Their findings were published in a recent paper in Translational Psychiatry.
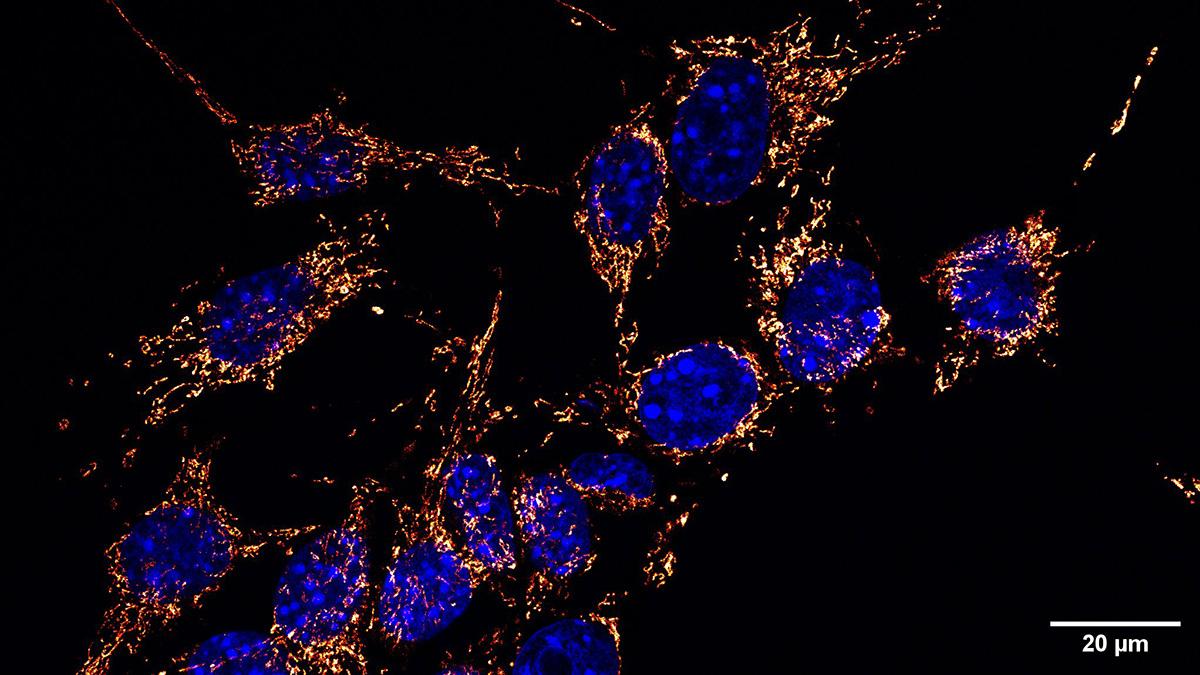
Fatigue is a common feature of major depressive disorder (MDD). The Cullen team wanted to better understand the origins of that fatigue to improve the quality of life of young MDD patients. To accomplish that, they compared ATP levels in cells from MDD patients and healthy controls. ATP levels were measured in brain cells by magnetic resonance spectroscopy and in peripheral blood mononuclear cells with a Seahorse instrument.
They found that the MDD patients had higher levels of ATP production than the controls, and those levels correlated positively with the measures of fatigue. In addition, those
This study is the first to show higher levels of ATP in brains and blood of MDD patients. The
findings suggest a compensatory mechanism early in the disease and may suggest strategies for future therapies.
A Conversation with Drs. Cullen and Tye
MitoWorld: Your discovery of a biosignature for fatigue in depressed youth is exciting. Can you give us an idea of where your research is going next? For example, do you plan to expand the sample size or to control for various drug treatments?
Cullen & Tye: Yes, we are actively seeking funding for this important work. Our hope is to confirm the findings from our paper in a larger group of young people. Controlling for medication can be a challenge due to ethical constraints, but it becomes more feasible with a large sample, to allow us to look at subgroups.
MitoWorld: The depression connection noted between your results and those for early Parkinson’s disease patients is interesting. It is reminiscent of the connection between early brain injury and Alzheimer’s disease. Do you have any thoughts on that?
Cullen & Tye: Given that depression is already an established risk factor for Alzheimer’s disease, we speculate that the bioenergetic signature we find could possibly represent a precursor reflecting physiological risk for dementia. If so, this biosignature could be a critical mechanistic link between the two conditions.
MitoWorld: Another recent paper showed a connection between mitochondrial health and depression. Could this be a common phenomenon? Do you think your findings would apply to muscle tissues?
Cullen & Tye: We suspect that impaired mitochondrial efficiency and capacity is likely to be reflected across all tissues. We are interested in the immune system as it is also closely linked to depression, as a mechanistic risk factor. The findings summarized in this review paper on mitochondrial health and inflammation in skeletal muscle hold potential relevance to depression, since the fatigue and low motivation in depression often contributes to sedentary behavior and muscle disuse. Taken together, an examination of mitochondrial health in muscle tissues in individuals with depression may be warranted.
MitoWorld: One of the mysteries that intrigue us is the “shared governance” of the mitochondrial and nuclear genomes. Do you have any speculation on how the nucleus signals to the mitochondria to increase the ATP levels in depression?
Cullen & Tye: This is a great question. The nucleus regulates mitochondrial ATP production indirectly through coordinated energy-sensing and transcriptional pathways, particularly via AMPK and PGC-1α, as well as rapid calcium and redox signaling that tune mitochondrial efficiency and capacity in real time. In depression, we speculate that this shared governance becomes dysregulated by chronic stress and immunometabolic adaptations to ongoing inflammatory load, resulting in the impairment of mitochondrial ATP production capacity to meet cellular demand.
MitoWorld: Do you think that your results might lead to clinical applications? For example, might the results from your MRI or PBMC studies might translate to a clinical test?
Cullen & Tye: Yes. While we are currently still in the foundational research stage, we strongly further stages of this research will have the potential to guide personalize clinical care. Part of the next steps include translating these findings to the clinic through biomarker-driven, companion diagnostic approaches.
Reference
Cullen KR, Tye SJ, Klimes-Dougan B, Wiesner HM, Varela RB, Morath B, Zhang L, Chen W, Zhu XH (2026) ATP bioenergetics and fatigue in young adults with and without major depression. Translational Psychiatry https://doi.org/10.1038/s41398-026-03904-y.