The Finley Lab
Context and Cell-State-Dependent Mitochondria Metabolic Pathway Engagement
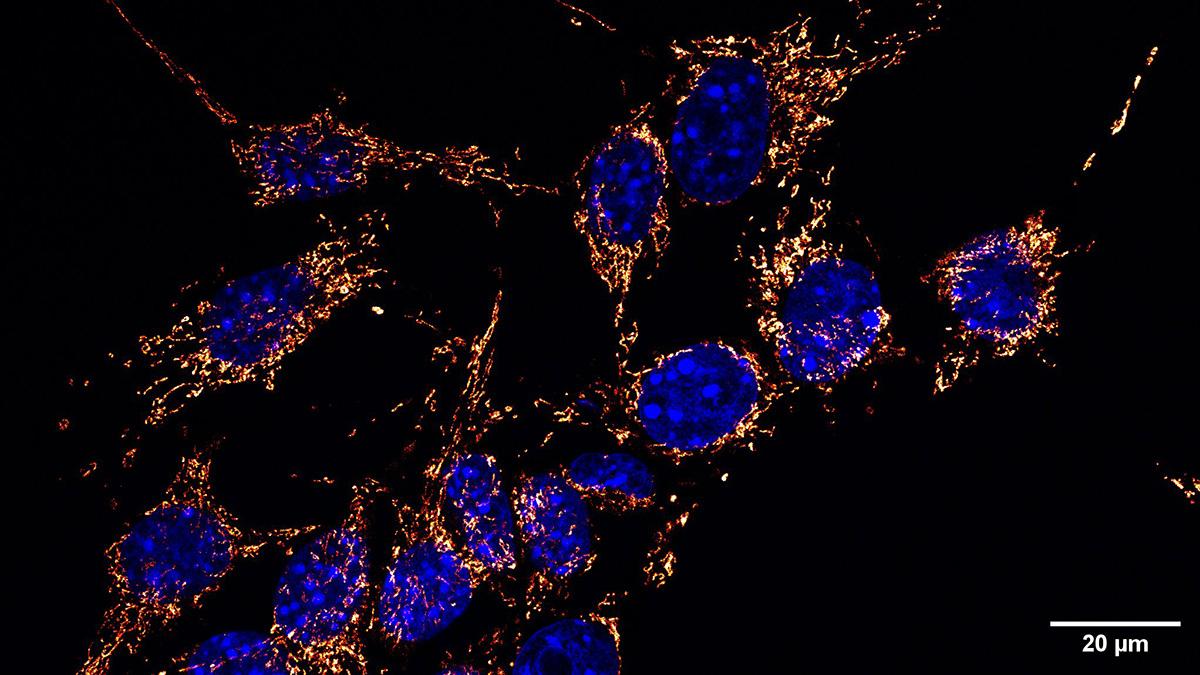
Mitochondria house metabolic pathways that support cell growth, survival, function and identity. Mutations in mitochondrial metabolic enzymes are drivers of many mitochondrial diseases, but different diseases arise when certain metabolic functions are disrupted, and the cell types affected are often poorly understood. In recent work published in Cell and Molecular Cell, a research team at Memorial Sloan Kettering Cancer Center, led by Abigail Xie, Julia Brunner and Lydia Finley shed light on when cells use different metabolic pathways within mitochondria and what essential functions are supported by mitochondrial metabolic networks.
The researchers focused on two related metabolic pathways that are required for importing nutrients into mitochondria and converting them into molecules that cells need to function. The tricarboxylic acid (TCA) cycle harnesses reducing equivalents from nutrients to fuel energy production in the electron transport chain (ETC), and the malate-aspartate shuttle transfers reducing equivalents from the cytosol to mitochondria for deposition onto the ETC. Despite the central role of these pathways within cellular metabolism, mammalian cells display surprising heterogeneity in whether, and how, they use these pathways. For example, some reactions of the TCA cycle can run in reverse or be skipped by exporting intermediates that are converted in the cytosol. The authors, therefore, set out to investigate the factors and contexts that dictate how the TCA cycle and related pathways are assembled in mammalian cells.
Reporting in Cell, co-first authors Xie and Brunner sought to determine what makes cells use the complete set of reactions that make up the “canonical” TCA cycle. They found that increasing cellular nutrient consumption by supplying cells with TCA cycle substrate pyruvate increased the production of citrate, the metabolite formed in the first step of the TCA cycle. Enhancing citrate production led to increased forward flux through the TCA cycle and induced dependence on enzyme aconitase 2, the TCA cycle enzyme that that breaks down citrate. To determine if aconitase 2 is also essential to break down citrate in vivo, they generated a mouse model of whole body, inducible aconitase 2 deficiency. Here, they discovered the kidney to be exquisitely sensitive to aconitase 2 loss. Notably, the kidney is unique for its ability to uptake and catabolize circulating citrate. The authors showed that cell autonomous citrate uptake is sufficient to induce reliance on aconitase 2 in cultured cells. Collectively, these results indicate that a major function of the TCA cycle is to remove citrate from mitochondria. This work demonstrates that apart from its known roles in nutrient breakdown and provision of metabolic intermediates, the TCA cycle is also important for metabolite clearance.
In the second study, the authors described how pathways that feed into the TCA cycle are differentially utilized depending on cell state. For cell metabolism to continually function, reducing equivalents generated in the cytosol must be transferred to mitochondria, where they can be safely deposited on the ETC. Reciprocally, oxidized intermediates generated within mitochondria must be delivered to the cytosol where they can be used to fuel biosynthetic pathways. One pathway, the malate-aspartate shuttle, fulfills both needs by transferring reduced nutrients (the TCA cycle intermediate malate) to mitochondria in exchange for aspartate. Mitochondrial production of aspartate is an essential function of the ETC in cultured cells. Here, the authors showed that the ability of aspartate to participate in the malate-aspartate shuttle and transfer reducing equivalents back into mitochondria depends on the relative balance between aspartate supply and demand within cells. Increasing or decreasing cytosolic aspartate levels with bacterial enzymes allowed cells to increase or decrease flux through the malate-aspartate shuttle, respectively. In turn, changing malate-aspartate shuttle flux changed how cells use metabolic pathways that depend on clearing reducing equivalents from the cytosol. Specifically, the ability to oxidize glucose required increased malate-aspartate flux. Accordingly, whereas proliferating cells with high aspartate demand had limited malate-aspartate shuttle flux and reduced glucose oxidation, differentiated cells with lower aspartate demand exhibited higher malate-aspartate shuttle flux that was sufficient to enable increased glucose oxidation—a metabolic hallmark of differentiated cells.
These findings illustrate how metabolic networks adopt different configurations depending on environmental context and cell state. Understanding when, and why, metabolic components become essential for different tissues and contexts will ultimately provide insight into the etiology of metabolic disease and nominate new approaches to target metabolism to manipulate cell states in cancer and other diseases.
A Statement of Significance from Dr. Lydia Finley
Mitochondria play critical roles converting nutrients into the molecules that cells need to function, but which metabolic pathways are used and which outputs are essential for cells are highly context-specific. For example, mutations in mitochondrial enzymes result in highly tissue-specific pathologies, indicating that different tissues—different cell types or cell states—have unique requirements for outputs of individual enzymes. In two papers, Brunner, Xie, and colleagues add to our understanding of how mitochondrial metabolic pathways are wired in to meet the demands of different cell contexts. In one study, they show that some cells depend on the TCA cycle not just to support energy production or anabolic synthesis but also to prevent metabolite accumulation within mitochondria. In another study, they show that as progenitor cells differentiate, they fully engage the malate-aspartate shuttle—an electron shuttle that enables cells to oxidize glucose within mitochondria. Together, these studies show how metabolic programs are wired to meet unique demands of different cell states. These studies support the argument that further identifying when and why metabolic enzymes are required will provide critical insight into how mitochondria support cell fitness and why mutations in mitochondrial genes lead to human disease.
A Conversation with Dr. Lydia Finely:
MitoWorld: How did you become interested in studying mitochondria? What interests you about them?
Dr. Finley: I became interested in metabolism as an undergraduate when I first learned that muscles can continually switch fuels to meet metabolic demands during exercise. This adaptability fascinated me, and I ended up working in a mitochondrial bioenergetics lab studying how mitochondria select different fuels to use during exercise and recovery from exercise. This adaptability fascinates me to this day: mitochondria are constantly sensing and responding to their surroundings and providing information about their decisions to the rest of the cell. They are like a little brain within a cell, taking in information and coordinating cellular responses.
MitoWorld: You mention that the kidney is uniquely sensitive to ACO2 deletion in the TCA cycle. Is that simply because it has to process so much citrate to remove it from circulation, or do you think there may be other reasons for this?
Dr. Finley: Likely many factors contribute to the importance of ACO2 in the kidney. We focused on the role of citrate uptake and showed that citrate uptake is sufficient to induce ACO2 dependence in non-kidney cells. That doesn’t rule out other functions of ACO2 in the kidney. Notably, the kidney proximal tubule cells, which displayed pathological abnormalities following ACO2 loss, are considered to be some of the most energy-demanding cells in the body. It will be interesting for future studies to determine whether this energy requirement contributes to ACO2 dependence in the kidney and, potentially, other organs.
MitoWorld: Other than the kidney, are there other types of cells or disease contexts that have unique characteristics or sensitivities when it comes to the TCA cycle? What does this tell you about them?
Dr. Finley: This is a major open question. Patients with ACO2 mutations often manifest with retinal phenotypes, suggesting that this cell type may have high reliance on ACO2. In cultured cancer cells, ACO2 is one of the most variably essential metabolic genes, meaning that some cells don’t care much about ACO2, while others do. What underlies this variability is a major question for us moving forward.
MitoWorld: The metabolic hallmark of differentiated cells with regard to the malate-aspartate shuttle is very interesting. Is this generally true of all types of differentiated cells, or are there some cell types that behave differently? Are there disease contexts where this changes, such as in cancer?
Dr. Finley: This is a great question. We’ve tested a few contexts where the transition from proliferative, progenitor to differentiated states shows this characteristic metabolic switch. How generalizable this switch is remains to be determined. Likely, some differentiated tissues will have specific metabolic requirements that push them to an alternate metabolic state. Continuing to identify how changes in cell state reorganize metabolism and which metabolic programs are required for certain cell states is a major area for future work.
MitoWorld: How might these pathways be targeted to treat disease, as you suggest in the conclusion? Through pharmaceuticals, through diet, other?
Dr. Finley: To know how to treat disease, we need to know why the disease arises. In many cases, mitochondrial diseases driven by the same genetic mutation affect different tissues (and even different people) differently. Why some tissues care more than others about specific mutations isn’t always clear. This variable dependence suggests that metabolic enzymes are required to meet needs that are specific to some tissues. If we can understand what these needs are—which metabolic outputs support essential functions in different tissues—we can better understand why pathologies emerge and, then, hopefully identify strategies to help tissues meet their specific needs and overturn these pathologies.
MitoWorld: What are the next steps for this research? What questions are you still trying to answer and why are they important?
Dr. Finley: We found that citrate accumulation within mitochondria activates a stress response known as the integrated stress response, which turns on genes that helps cells adapt to stress or other environmental changes. We are working to understand how mitochondrial citrate, or consequences of citrate accumulation within mitochondria, turn on a cytoplasmic stress response. We hope these studies will provide new insight into how changes within mitochondria are communicated throughout the cell to help cells adapt and respond to changes in mitochondrial activity.
MitoWorld: Anything else you think the audience should know?
Dr. Finley: Metabolism is not one-size-fits-all. It highly, highly variable, and there is a lot left to learn about cell metabolism!
References:
Abigail Xie, Julia S Brunner, Sangita Chakraborty, Angela M Montero, Anna E Bridgeman, Katrina I Paras, Ruobing Cui, Maider Fagoaga-Eugui, Monika Komza, Paige K Arnold, Benjamin T Jackson, Santiago Noriega Madrazo, Mohamed I Atmane, Sebastian E Carrasco, Lydia W S Finley (2026) Citrate clearance is a major function of aconitase 2 in the canonical TCA cycle. Cell 189(9):2684-2699.e21.